Diabetes mellitus, often simply referred to as
diabetes—is a group of metabolic diseases in which a person has high
blood sugar, either because the body does not produce enough
insulin, or because cells do not respond to the insulin that is produced. This high blood sugar produces the classical symptoms of
polyuria (frequent urination),
polydipsia (increased thirst) and
polyphagia (increased hunger).
There are three main types of diabetes:
- Type 1 diabetes: results from the body's failure to produce insulin, and presently requires the person to inject insulin. (Also referred to as insulin-dependent diabetes mellitus, IDDM for short, and juvenile diabetes.)
- Type 2 diabetes: results from insulin resistance, a condition in which cells fail to use insulin properly, sometimes combined with an absolute insulin deficiency. (Formerly referred to as non-insulin-dependent diabetes mellitus, NIDDM for short, and adult-onset diabetes.)
- Gestational diabetes: is when pregnant women, who have never had diabetes before, have a high blood glucose level during pregnancy. It may precede development of type 2 DM.
Other forms of diabetes mellitus include congenital diabetes, which is due to genetic defects of insulin secretion, cystic fibrosis-related diabetes, steroid diabetes induced by high doses of glucocorticoids, and several forms of
monogenic diabetes.
All forms of diabetes have been treatable since
insulin became available in 1921, and type 2 diabetes may be controlled with medications. Both type 1 and 2 are
chronic conditions that usually cannot be cured.
Pancreas transplants have been tried with limited success in type 1 DM;
gastric bypass surgery has been successful in many with
morbid obesity and type 2 DM. Gestational diabetes usually resolves after delivery. Diabetes without proper treatments can cause many complications.
Acute complications include
hypoglycemia,
diabetic ketoacidosis, or
nonketotic hyperosmolar coma. Serious long-term complications include
cardiovascular disease,
chronic renal failure,
retinal damage. Adequate treatment of diabetes is thus important, as well as
blood pressure control and lifestyle factors such as
smoking cessation and maintaining a healthy
body weight.
As of 2000 at least 171 million people worldwide suffer from diabetes, or 2.8% of the population.
[2] Type 2 diabetes is by far the most common, affecting 90 to 95% of the U.S. diabetes population.
[3]DefinitionThe term
diabetes, without qualification, usually refers to diabetes mellitus, which roughly translates to excessive sweet urine (known as "
glycosuria"). Several rare conditions are also named diabetes. The most common of these is
diabetes insipidus in which large amounts of urine are produced (
polyuria), which is not sweet (insipidus meaning "without taste" in Latin).
The term "type 1 diabetes" has replaced several former terms, including childhood-onset diabetes, juvenile diabetes, and insulin-dependent diabetes mellitus (IDDM). Likewise, the term "type 2 diabetes" has replaced several former terms, including adult-onset diabetes, obesity-related diabetes, and non-insulin-dependent diabetes mellitus (NIDDM). Beyond these two types, there is no agreed-upon standard nomenclature. Various sources have defined "type 3 diabetes" as:
gestational diabetes,
[4] insulin-resistant type 1 diabetes (or "double diabetes"), type 2 diabetes which has progressed to require injected insulin, and
latent autoimmune diabetes of adults (or LADA or "
type 1.5" diabetes)
[5]ClassificationMost cases of diabetes mellitus fall into three broad categories:
type 1,
type 2, and
gestational diabetes. A few other types are described.
Type 1 diabetesMain article:
Diabetes mellitus type 1Type 1 diabetes mellitus is characterized by loss of the insulin-producing
beta cells of the
islets of Langerhans in the pancreas leading to insulin deficiency. This type of diabetes can be further classified as immune-mediated or idiopathic. The majority of type 1 diabetes is of the immune-mediated nature, where beta cell loss is a
T-cell mediated
autoimmune attack.
[6] There is no known preventive measure against type 1 diabetes, which causes approximately 10% of diabetes mellitus cases in North America and Europe. Most affected people are otherwise healthy and of a healthy weight when onset occurs. Sensitivity and responsiveness to insulin are usually normal, especially in the early stages. Type 1 diabetes can affect children or adults but was traditionally termed "juvenile diabetes" because it represents a majority of the diabetes cases in children.
Type 2 diabetesMain article:
Diabetes mellitus type 2Type 2 diabetes mellitus is characterized by
insulin resistance which may be combined with relatively reduced insulin secretion. The defective responsiveness of body tissues to insulin is believed to involve the
insulin receptor. However, the specific defects are not known. Diabetes mellitus due to a known defect are classified separately. Type 2 diabetes is the most common type.
In the early stage of type 2 diabetes, the predominant abnormality is reduced insulin sensitivity. At this stage hyperglycemia can be reversed by a variety of measures and
medications that improve insulin sensitivity or reduce glucose production by the
liver.
Gestational diabetesMain article:
Gestational diabetesGestational diabetes mellitus (GDM) resembles type 2 diabetes in several respects, involving a combination of relatively inadequate insulin secretion and responsiveness. It occurs in about 2%–5% of all
pregnancies and may improve or disappear after delivery. Gestational diabetes is fully treatable but requires careful medical supervision throughout the pregnancy. About 20%–50% of affected women develop type 2 diabetes later in life.
Even though it may be transient, untreated gestational diabetes can damage the health of the fetus or mother. Risks to the baby include
macrosomia (high birth weight), congenital cardiac and central nervous system anomalies, and skeletal muscle malformations. Increased fetal insulin may inhibit fetal
surfactant production and cause
respiratory distress syndrome.
Hyperbilirubinemia may result from red blood cell destruction. In severe cases, perinatal death may occur, most commonly as a result of poor placental perfusion due to vascular impairment.
Labor induction may be indicated with decreased placental function. A
cesarean section may be performed if there is marked fetal distress or an increased risk of injury associated with
macrosomia, such as
shoulder dystocia.
A 2008 study completed in the U.S. found that the number of American women entering pregnancy with preexisting diabetes is increasing. In fact the rate of diabetes in expectant mothers has more than doubled in the past 6 years.
[7] This is particularly problematic as diabetes raises the risk of complications during pregnancy, as well as increasing the potential that the children of diabetic mothers will also become diabetic in the future.
Other typesPre-diabetes indicates a condition that occurs when a person's blood glucose levels are higher than normal but not high enough for a diagnosis of type 2 diabetes. Many people destined to develop type 2 diabetes spend many years in a state of pre-diabetes which has been termed "America's largest healthcare epidemic."
[8]:10–11Some cases of diabetes are caused by the body's tissue receptors not responding to insulin (even when insulin levels are normal, which is what separates it from type 2 diabetes); this form is very uncommon. Genetic mutations (
autosomal or
mitochondrial) can lead to defects in beta cell function. Abnormal insulin action may also have been genetically determined in some cases. Any disease that causes extensive damage to the pancreas may lead to diabetes (for example,
chronic pancreatitis and
cystic fibrosis). Diseases associated with excessive secretion of insulin-antagonistic hormones can cause diabetes (which is typically resolved once the hormone excess is removed). Many drugs impair insulin secretion and some toxins damage pancreatic beta cells. The
ICD-10 (1992) diagnostic entity,
malnutrition-related diabetes mellitus (MRDM or MMDM, ICD-10 code E12), was deprecated by the
World Health Organization when the current taxonomy was introduced in 1999.
[9]Following is a comprehensive list of other causes of diabetes:
[10]Signs and symptoms

Overview of the most significant symptoms of diabetes.
The classical symptoms of diabetes are
polyuria (frequent urination),
polydipsia (increased thirst) and
polyphagia (increased hunger).
[11] Symptoms may develop rapidly (weeks or months) in type 1 diabetes while in type 2 diabetes they usually develop much more slowly and may be subtle or absent.
Prolonged high blood glucose causes glucose absorption, which leads to changes in the shape of the lenses of the eyes, resulting in vision changes; sustained sensible glucose control usually returns the lens to its original shape. Blurred vision is a common complaint leading to a diabetes diagnosis; type 1 should always be suspected in cases of rapid vision change, whereas with type 2 change is generally more gradual, but should still be suspected.
People (usually with type 1 diabetes) may also present with
diabetic ketoacidosis, a state of metabolic dysregulation characterized by the smell of
acetone; a rapid, deep breathing known as
Kussmaul breathing; nausea; vomiting and
abdominal pain; and an altered states of consciousness.
A rarer but equally severe possibility is
hyperosmolar nonketotic state, which is more common in type 2 diabetes and is mainly the result of dehydration. Often, the patient has been drinking extreme amounts of sugar-containing drinks, leading to a
vicious circle in regard to the water loss.
A number of skin rashes can occur in diabetes that are collectively known as
diabetic dermadromes.
CausesThe cause of diabetes depends on the type. Type 2 diabetes is due primarily to lifestyle factors
[clarification needed] and genetics.
[12]Type 1 diabetes is also partly inherited and then triggered by certain infections, with some evidence pointing at
Coxsackie B4 virus. There is a genetic element in individual susceptibility to some of these triggers which has been traced to particular
HLA genotypes (i.e., the genetic "self" identifiers relied upon by the immune system). However, even in those who have inherited the susceptibility, type 1 diabetes mellitus seems to require an environmental trigger.
Pathophysiology

The fluctuation of blood sugar (red) and the sugar-lowering hormone
insulin (blue) in humans during the course of a day with three meals. One of the effects of a
sugar-rich vs a
starch-rich meal is highlighted.


Mechanism of insulin release in normal pancreatic beta cells. Insulin production is more or less constant within the beta cells, irrespective of blood glucose levels. It is stored within vacuoles pending release, via exocytosis, which is primarily triggered by food, chiefly food containing absorbable glucose. The chief trigger is a rise in blood glucose levels after eating
Insulin is the principal hormone that regulates uptake of
glucose from the blood into most cells (primarily muscle and fat cells, but not central nervous system cells). Therefore deficiency of insulin or the insensitivity of its
receptors plays a central role in all forms of diabetes mellitus.
Humans are capable of digesting some
carbohydrates, in particular those most common in food; starch, and some disaccharides such as sucrose, are converted within a few hours to simpler forms most notably the
monosaccharide glucose, the principal carbohydrate energy source used by the body. The rest are passed on for processing by gut flora largely in the colon. Insulin is released into the blood by beta cells (β-cells), found in the Islets of Langerhans in the pancreas, in response to rising levels of blood glucose, typically after eating. Insulin is used by about two-thirds of the body's cells to absorb glucose from the blood for use as fuel, for conversion to other needed molecules, or for storage.
Insulin is also the principal control signal for conversion of glucose to
glycogen for internal storage in liver and muscle cells. Lowered glucose levels result both in the reduced release of insulin from the beta cells and in the reverse conversion of glycogen to glucose when glucose levels fall. This is mainly controlled by the hormone
glucagon which acts in the opposite manner to insulin. Glucose thus forcibly produced from internal liver cell stores (as glycogen) re-enters the bloodstream; muscle cells lack the necessary export mechanism. Normally liver cells do this when the level of insulin is low (which normally correlates with low levels of blood glucose).
Higher insulin levels increase some
anabolic ("building up") processes such as cell growth and duplication,
protein synthesis, and
fat storage. Insulin (or its lack) is the principal signal in converting many of the bidirectional processes of metabolism from a
catabolic to an anabolic direction, and vice versa. In particular, a low insulin level is the trigger for entering or leaving ketosis (the fat burning metabolic phase).
If the amount of insulin available is insufficient, if cells respond poorly to the effects of insulin (insulin insensitivity or
resistance), or if the insulin itself is defective, then glucose will not have its usual effect so that glucose will not be absorbed properly by those body cells that require it nor will it be stored appropriately in the liver and muscles. The net effect is persistent high levels of blood glucose, poor protein synthesis, and other metabolic derangements, such as
acidosis.
When the glucose concentration in the blood is raised beyond its
renal threshold (about 10 mmol/L, although this may be altered in certain conditions, such as pregnancy),
reabsorption of glucose in the
proximal renal tubuli is incomplete, and part of the glucose remains in the
urine (
glycosuria). This increases the
osmotic pressure of the urine and inhibits reabsorption of water by the kidney, resulting in increased urine production (
polyuria) and increased fluid loss. Lost blood volume will be replaced osmotically from water held in body cells and other body compartments, causing
dehydration and increased thirst.
DiagnosisSee also:
Glycosylated hemoglobin and
Glucose tolerance test2006 WHO Diabetes criteria[13] editCondition2 hour glucoseFasting glucose
| mmol/l(mg/dl) | mmol/l(mg/dl) |
| Normal | <7.8 (<140) | <6.1 (<110) |
| Impaired fasting glycaemia | <7.8 (<140) | ≥ 6.1(≥110) & <7.0(<126) |
| Impaired glucose tolerance | ≥7.8 (≥140) | <7.0 (<126) |
| Diabetes mellitus | ≥11.1 (≥200) | ≥7.0 (≥126) |
Diabetes mellitus is characterized by recurrent or persistent hyperglycemia, and is diagnosed by demonstrating any one of the following:
[9]A positive result, in the absence of unequivocal hyperglycemia, should be confirmed by a repeat of any of the above-listed methods on a different day. It is preferable to measure a fasting glucose level because of the ease of measurement and the considerable time commitment of formal glucose tolerance testing, which takes two hours to complete and offers no prognostic advantage over the fasting test.
[15] According to the current definition, two fasting glucose measurements above 126 mg/dL (7.0 mmol/L) is considered diagnostic for diabetes mellitus.
People with fasting glucose levels from 100 to 125 mg/dL (5.6 to 6.9 mmol/L) are considered to have
impaired fasting glucose. Patients with plasma glucose at or above 140 mg/dL (7.8 mmol/L), but not over 200 mg/dL (11.1 mmol/L), two hours after a 75 g oral glucose load are considered to have
impaired glucose tolerance. Of these two pre-diabetic states, the latter in particular is a major risk factor for progression to full-blown diabetes mellitus as well as cardiovascular disease.
[16]ManagementMain article:
Diabetes managementDiabetes mellitus is a
chronic disease which is difficult to cure. Management concentrates on keeping blood sugar levels as close to normal ("euglycemia") as possible without presenting undue patient danger. This can usually be with close dietary management, exercise, and use of appropriate medications (insulin only in the case of type 1 diabetes mellitus. Oral medications may be used in the case of type 2 diabetes, as well as insulin).
Patient education, understanding, and participation is vital since the complications of diabetes are far less common and less severe in people who have well-managed blood sugar levels.
[17][18] Wider health problems may accelerate the deleterious effects of diabetes. These include
smoking,
elevated cholesterol levels,
obesity,
high blood pressure, and lack of regular
exercise.
Lifestyle modificationsMain article:
Diabetic dietThere are roles for patient education, dietetic support, sensible exercise, with the goal of keeping both short-term and long-term blood glucose levels
within acceptable bounds. In addition, given the associated higher risks of cardiovascular disease, lifestyle modifications are recommended to control blood pressure.
[19]MedicationsOral medications Main article:
Anti-diabetic drugRoutine use of
aspirin has not been found to improve outcomes in uncomplicated diabetes.
[20]Insulin Main article:
Insulin therapyType 1 treatments usually include combinations of regular or NPH insulin, and/or synthetic insulin analogs.
SupportIn countries using a
general practitioner system, such as the
United Kingdom, care may take place mainly outside hospitals, with hospital-based specialist care used only in case of complications, difficult blood sugar control, or research projects. In other circumstances, general practitioners and specialists share care of a patient in a team approach.
Optometrists,
podiatrists/chiropodists,
dietitians,
physiotherapists, nursing specialists (e.g., DSNs (Diabetic Specialist Nurse)),
nurse practitioners, or
Certified Diabetes Educators, may jointly provide multidisciplinary expertise. In countries where patients must provide for their own health care (e.g. in the US, and in much of the undeveloped world).
Peer support links people living with diabetes. Within peer support, people with a common illness share knowledge and experience that others, including many health workers, do not have. Peer support is frequent, ongoing, accessible and flexible and can take many forms—phone calls, text messaging, group meetings, home visits, and even grocery shopping. It complements and enhances other health care services by creating the emotional, social and practical assistance necessary for managing disease and staying healthy.
PrognosisMain article:
Prognosis of diabetes mellitusDiabetes doubles the risk of vascular problems, including
cardiovascular disease.
[21]According to one study, women with high blood pressure (hypertension) were three times more likely to develop type 2 diabetes as compared with women with optimal BP after adjusting for various factors such as age, ethnicity, smoking, alcohol intake, body mass index (BMI), exercise, family history of diabetes, etc.
[22] The study was conducted by researchers from the
Brigham and Women’s Hospital,
Harvard Medical School and the
Harvard School of Public Health, USA, who followed over 38,000 female health professionals for ten years.
Except in the case of type 1 diabetes, which always requires insulin replacement, the way type 2 diabetes is managed may change with age. Insulin production decreases because of age-related impairment of pancreatic beta cells. Additionally, insulin resistance increases because of the loss of lean tissue and the accumulation of fat, particularly intra-abdominal fat, and the decreased tissue sensitivity to insulin. Glucose tolerance progressively declines with age, leading to a high prevalence of type 2 diabetes and postchallenge hyperglycemia in the older population.
[23] Age-related glucose intolerance in humans is often accompanied by insulin resistance, but circulating insulin levels are similar to those of younger people.
[24] Treatment goals for older patients with diabetes vary with the individual, and take into account health status, as well as life expectancy, level of dependence, and willingness to adhere to a treatment regimen.
[25] Glycated hemoglobin is better than
fasting glucose for determining risks of cardiovascular disease and death from any cause.
[26]Epidemiology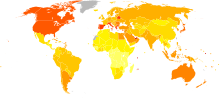

Prevalence of diabetes worldwide in 2000 (per 1000 inhabitants). World average was 2.8%. no data ≤ 7.5 7.5–15 15–22.5 22.5–30 30–37.5 37.5–45 45–52.5 52.5–60 60–67.5 67.5–75 75–82.5 ≥ 82.5

 Disability-adjusted life year
Disability-adjusted life year for diabetes mellitus per 100,000 inhabitants in 2002.
[27] no data ≤ 100 100-200 200-300 300-400 400-500 500-600 600-700 700-800 800-900 900-1000 1000-1500 ≥ 1500
In 2000, according to the World Health Organization, at least 171 million people worldwide suffer from diabetes, or 2.8% of the population.
[2] Its incidence is increasing rapidly, and it is estimated that by 2030, this number will almost double.
[2] Diabetes mellitus occurs throughout the world, but is more common (especially type 2) in the more developed countries. The greatest increase in prevalence is, however, expected to occur in Asia and Africa, where most patients will probably be found by 2030.
[2] The increase in incidence of diabetes in developing countries follows the trend of urbanization and lifestyle changes, perhaps most importantly a "Western-style" diet. This has suggested an environmental (i.e., dietary) effect, but there is little understanding of the mechanism(s) at present, though there is much speculation, some of it most compellingly presented.
[2]For at least 20 years, diabetes rates in North America have been increasing substantially. In 2008 there were about 24 million people with diabetes in the United States alone, from those 5.7 million people remain undiagnosed. Other 57 million people are estimated to have pre-diabetes.
[28]The
Centers for Disease Control has termed the change an
epidemic.
[29] The
National Diabetes Information Clearinghouse estimates that diabetes costs $132 billion in the United States alone every year. About 5%–10% of diabetes cases in North America are type 1, with the rest being type 2. The fraction of type 1 in other parts of the world differs. Most of this difference is not currently understood. The American Diabetes Association cite the 2003 assessment of the National Center for Chronic Disease Prevention and Health Promotion (Centers for Disease Control and Prevention) that 1 in 3 Americans born after 2000 will develop diabetes in their lifetime.
[30][31]According to the American Diabetes Association, approximately 18.3% (8.6 million) of Americans age 60 and older have diabetes.
[32] Diabetes mellitus prevalence increases with age, and the numbers of older persons with diabetes are expected to grow as the elderly population increases in number. The National Health and Nutrition Examination Survey (NHANES III) demonstrated that, in the population over 65 years old, 18% to 20% have diabetes, with 40% having either diabetes or its precursor form of
impaired glucose tolerance.
[23]Indigenous populations in first world countries have a higher prevalence and increasing incidence of diabetes than their corresponding non-indigenous populations. In Australia the age-standardised prevalence of self-reported diabetes in Indigenous Australians is almost 4 times that of non-indigenous Australians.
[33] Preventative community health programs such as
Sugar Man (diabetes education) are showing some success in tackling this problem.

